(Curse or Boon? Understanding the Double Life of the Vagus Nerve)
Most people talk about stress, hormones, or lifestyle when their body feels “off.”
But some of us live with something deeper — a hidden nervous-system disorder where blood pressure shoots up without warning, spice or heat becomes unbearable, migraines arrive like clockwork, and even the smallest emotional trigger sends the body into chaos.
This condition has a name: Vagal Dysautonomia.
And here is the strange part — while it makes daily life difficult, it also slows visible aging.
People with this condition often look 10–15 years younger than their real age.
So… is vagal dysautonomia a curse or a biological accident that also brings a secret gift?
Let’s break it down simply.
What Is Vagal Dysautonomia?
The vagus nerve is the body’s master regulator.
It controls:
- Heart rate
- Blood pressure
- Digestion
- Inflammation
- Stress response
- Cooling and temperature tolerance
- Emotional regulation
In dysautonomia, this system becomes unstable:
- At one moment the vagus nerve is too active → causing low BP, dizziness, nausea.
- Next moment it withdraws suddenly → BP spikes to 160–180, chest pressure, panic-like waves.
It feels like the body has “no buffer” between calm and chaos.
What Living With Dysautonomia Feels Like
Dysautonomia can look very different for every person. Even two people in the same family may have completely different symptoms. Some might struggle with dizziness, some with fatigue, and others with stomach issues or heart rate changes. Because it varies so much, getting a clear diagnosis can take time. It’s normal to feel confused, frustrated, or anxious when your body behaves unpredictably. Many people with dysautonomia experience these same emotions—you’re not alone in this.
Is Dysautonomia Temporary or Lifelong?
For some people, dysautonomia appears during illness, infection, or stress and improves once the body heals. But in many cases, it stays for a long time. Most forms tend to be chronic, meaning they don’t go away completely and need ongoing care and understanding.
Understanding the Long-Term Outlook
The course of dysautonomia is not easy to predict. Some people have symptoms almost every day. Others may feel normal for months or years before symptoms return. Your doctor can help you understand what is likely for your specific situation and how to reduce the impact on your daily life. Small changes—like pacing, hydration, or managing stress—can make a big difference.
When Dysautonomia Becomes More Serious
For many people, dysautonomia is manageable and only mildly affects daily life. But when it is caused by chronic or incurable conditions, it can have a bigger impact. In severe cases, symptoms may interfere with work, socializing, or hobbies you once enjoyed. Rarely, serious complications can occur. That’s why ongoing medical guidance, self-care, and paying attention to your body’s signals are so important.
Primary vs. Secondary Vagal Dysautonomia
Vagal dysautonomia appears in two forms. Primary vagal dysautonomia is built into a person’s nervous system from early life — often seen in people with childhood migraines, high sensitivity, or naturally unstable autonomic circuits. Their vagus nerve overreacts or withdraws suddenly without any external medical cause. In contrast, secondary vagal dysautonomia develops due to an underlying trigger such as heat stress, chronic inflammation, trauma, infections, metabolic issues, or MTHFR-related detox problems. Here the vagus becomes unstable because another condition is stressing the system. Understanding whether your dysautonomia is primary or secondary helps guide treatment, diet choices, and long-term management.
What Causes Vagal Dysautonomia?
1. Long-term fight-or-flight living
Years of emotional stress, survival mode, or unsafe environments exhaust the sympathetic system → vagus becomes hypersensitive.
2. Heat stress / sun exposure in summer
Extreme heat overstimulates the brainstem → vagal collapse → BP swings.
3. Childhood migraine brain
Migraine-prone individuals have sensitive brainstem pathways and unstable autonomic responses.
4. MTHFR mutation
Leads to inflammation, poor detox, and hypersensitive nerves.
5. Spices & alkaloids
Capsaicin, ginger, fenugreek, ajwain overstimulate vagal sensory fibers → migraines + BP changes.
6. Poor blood sugar stability
Low or fluctuating glucose triggers sympathetic surges → worsens vagal instability.
Classic Symptoms
1. Blood pressure swings
- BP rising from 120 to 170–180 within minutes
- Sudden drops with emotions (thinking of someone you love, pets, calm memories)
2. Chest pressure with stress
Not a heart issue — a vagus withdrawal reaction.
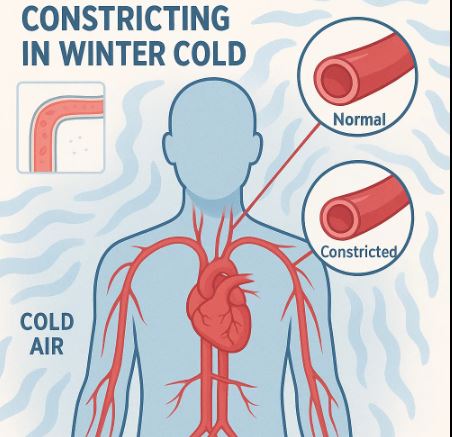
3. Heat intolerance
Sun, hot showers, summer afternoons = instant migraine, fatigue, or BP rise.
4. “Brain feels inflamed” feeling
Burning behind eyes, forehead pressure, or neck heat.
5. Spice intolerance
Even slight chilli → migraine, nausea, heart pounding.
6. Random episodes of restlessness
A sudden “internal electricity” feeling without any emotional reason.
7. Youthful appearance
Slow aging due to low cortisol spikes and high serotonin sensitivity.
Skin stays smooth, tight, and youthful.
Common Triggers of Vagal Dysautonomia
- Heat (sunlight, summer months)
- Hunger / low blood sugar
- Overthinking or sudden stress
- Coffee
- Chilli / capsicum / ginger / fenugreek
- Dehydration
- Loud noises or bright light
- Sudden emotional memories
- Overexercise or high-intensity workouts
Is It a Curse or a Boon?
The Curse:
- Constant internal instability
- Sensitivity to heat, spices, stress
- BP spikes + migraines
- Exhaustion after emotional triggers
The Boon:
- High vagal sensitivity reduces chronic cortisol
- Lower oxidative stress → slower aging
- Sharper intuition, deeper emotional perception
- Naturally youthful face for decades
It is both — a difficult disorder wrapped inside unexpected biological protection.
How to Calm Vagal Dysautonomia
1. Diet (The most powerful tool)
Eat foods that stabilize sugar + calm inflammation:
Best foods:
- Rice
- Oats
- Bananas
- Tender coconut
- Coconut water
- Boiled potatoes
- Ghee
- Curd (if tolerable)
- Sweet fruits (mango, grapes, chiku)
- Milk with jaggery
Avoid:
- Chilli
- Ajwain
- Ginger
- Fenugreek
- Coffee
- Bitter foods
They trigger autonomic storms.
2. Workouts
Avoid high-intensity anything.
Choose slow, vagus-friendly movement:
- Light walking
- Yoga (especially forward bends)
- Cycling indoors
- Swimming (cooling effect)
- Stretching
- Slow dancing
Never exercise in heat.
3. Vagus-Stabilizing Daily Practices
- 4–8 breathing: inhale 4 sec → exhale 8 sec
- No long gaps between meals
- Consistent sleep timing
- Cooling the neck with a wet cloth
- Cold water face splash
- Magnesium before bed
These keep the vagus “steady” instead of overreacting.
4. Summer Protection Plan
This is crucial
- Avoid outdoor heat 9 AM–5 PM
- Drink ORS or electrolyte water daily
- Keep wet cloth on neck while working
- Use cooling showers
- Stay in shaded/air-conditioned environments
- Increase fruits and fluids in May–June
This prevents the dangerous vagal collapses that cause BP spikes.
Final Thought
Vagal dysautonomia makes life more sensitive — emotionally and physically.
But with the right understanding, lifestyle, and diet, it becomes manageable.
And the silver lining is undeniable:
Your body may struggle…
but your face and energy age slowly, gracefully, almost mysteriously.
It is a fragile gift — and a demanding teacher.