
With winters around the corner in South Asia and as the temperatures drop, a surprising number of people start experiencing an odd winter ritual: fingers that turn numb, stiff, or icy cold, even when the rest of the body feels warm.
Raynaud’s syndrome—also called Raynaud’s phenomenon—is a condition in which certain parts of the body, usually the fingers and toes, temporarily lose blood flow when exposed to cold or emotional stress. During an episode, the affected areas may feel numb, cold, or painful. While many people know Raynaud’s for its classic color changes (white → blue → red), not everyone experiences these colors, especially those with deeper skin tones or milder symptoms. For many, the signs are subtle—like tingling, heaviness, or temporary numbness in specific fingers.
Raynaud’s is more common than most people realize, and early awareness helps people manage symptoms before they become severe. This article explains the two types of Raynaud’s, its causes, symptoms, treatment options, and the precautions needed to prevent attacks.
What Is Raynaud’s Syndrome?
Raynaud’s syndrome is a disorder where the small blood vessels in the fingers, toes, or other body parts suddenly narrow (called vasospasm). When this happens, blood flow temporarily reduces, leading to numbness, coldness, or color change.
There are two main types:
1. Primary Raynaud’s
This is the most common type.
It occurs on its own and is usually mild. People often notice symptoms during winter or when touching cold objects.
2. Secondary Raynaud’s
This form is less common but more serious.
It occurs due to an underlying medical condition—most often autoimmune or connective tissue diseases like lupus, rheumatoid arthritis, or scleroderma. Secondary Raynaud’s can cause more intense symptoms and sometimes finger ulcers.
What Causes Raynaud’s Syndrome?
The exact reason why the blood vessels overreact is not fully known, but several factors contribute.
In primary Raynaud’s, the cause is mostly functional.
In secondary Raynaud’s, the reasons are linked to diseases that affect blood vessels or the immune system.
Common causes include:
- Cold exposure (winter air, refrigerator use, holding cold objects)
- Emotional stress
- Autoimmune diseases like lupus, scleroderma, Sjögren’s
- Repetitive vibration exposure (jackhammers, machinery)
- Smoking (reduces blood flow)
- Certain medications such as beta-blockers or decongestants
- Injuries to hands or fingers
- Hormonal and circulatory imbalances
How Many People Have Raynaud’s?
Raynaud’s is surprisingly common worldwide. Studies suggest that:
- 3–5% of the general population has Raynaud’s.
- It is more common in women than men.
- Primary Raynaud’s usually begins between age 15–30.
- Secondary Raynaud’s often appears after age 30.
Because symptoms vary and are often ignored, many people live with Raynaud’s without ever getting diagnosed.
Symptoms of Raynaud’s Syndrome
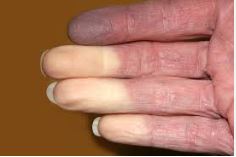
Raynaud’s affects the body in episodes called “attacks.” These attacks can last from a few minutes to over an hour.
The most common symptoms include:
- Coldness, numbness, or tingling in fingers or toes
- Reduced feeling or heaviness in affected areas
- Color changes (not always present):
- White (blood flow stops)
- Blue (lack of oxygen)
- Red (blood returns)
- Pins-and-needles sensation when the blood flow comes back
- Pain or throbbing after warming
- Symptoms triggered by cold or stress
- Sometimes affects ears, nose, lips, or one hand more than the other
Not everyone has full color changes. Some people only feel numbness, stiffness, or coldness in one or two fingers.
Treatment Options
Raynaud’s treatment focuses on improving blood flow, reducing attacks, and preventing complications. Most people with primary Raynaud’s manage well with simple lifestyle adjustments.
Lifestyle Management (First Choice for Most People)
- Keep hands, feet, and whole body warm
- Wear insulated gloves, wool socks, hats, and warm layers
- Avoid sudden temperature changes
- Manage emotional stress through breathing exercises or mindfulness
- Stop smoking
- Regular exercise to improve circulation
Medications (For Moderate to Severe Symptoms)
Doctors may prescribe:
- Calcium channel blockers (nifedipine, amlodipine) – first-line treatment
- Vasodilators such as sildenafil or topical nitroglycerin
- Drugs that relax blood vessels in severe cases
- Treatment of underlying disease if secondary Raynaud’s is suspected
If the Raynaud’s is secondary, managing the underlying condition is extremely important.
Precautions to Reduce Attacks
Small lifestyle habits can significantly reduce the frequency and severity of Raynaud’s episodes.
Helpful precautions include:
- Avoid cold exposure; keep gloves handy even indoors
- Warm the hands before entering cold environments
- Never place hands directly into cold water
- Reduce caffeine and nicotine
- Maintain good hydration
- Avoid tight rings or wristbands that restrict circulation
- Be cautious with medications that constrict blood vessels
- Keep stress levels low using yoga, meditation, or simple deep breaths
For secondary Raynaud’s, regular checkups are important to monitor any underlying condition.
Final Thoughts
Raynaud’s syndrome may seem harmless at first—just cold or numb fingers—but understanding the symptoms helps prevent long-term problems. Most people with primary Raynaud’s lead normal lives with simple adjustments. However, symptoms that appear in only one hand, begin after age 30, or include severe pain or ulcers should be evaluated by a doctor to rule out secondary causes.
If you or someone you know experiences winter numbness, tingling, or cold fingers, reading about this condition can help them understand what might be happening and when to seek medical guidance.